Esketamine Side Effect Tracker
Blood Pressure Monitor
Dissociation Tracker
0 (None)
10 (Severe)
Treatment Monitoring Timeline
Before Treatment
0 minutes
During Treatment (Peak at ~40 min)
40 minutes
After Treatment (2 hours total)
120 minutes
When traditional antidepressants fail, esketamine nasal spray-marketed as Spravato-offers a lifeline. But it’s not like taking a daily pill. This treatment comes with intense side effects, strict rules, and a monitoring system unlike anything else in depression care. If you or someone you know is considering esketamine, understanding what happens during and after each dose isn’t optional-it’s essential.
How Esketamine Works (And Why It’s Different)
Most antidepressants target serotonin, norepinephrine, or dopamine. Esketamine doesn’t. Instead, it blocks NMDA receptors in the brain, which are part of the glutamate system. This is a completely different pathway. Think of it like rerouting traffic: while other drugs tweak mood chemicals slowly, esketamine triggers a rapid cascade of neural activity. That’s why some patients feel better within hours, not weeks. It’s not magic. It’s science. And that science comes with side effects that can’t be ignored. The most common? Dissociation and spikes in blood pressure. These aren’t rare blips-they’re expected, predictable, and carefully managed.Dissociation: Feeling Unreal, But Not Alone
If you’ve ever heard someone describe esketamine as making them feel “like they’re in a dream,” they’re not exaggerating. In clinical trials, over half of patients (56.2%) experienced dissociation during their first few treatments. That’s more than four times higher than placebo. Symptoms vary. Some feel detached from their body. Others say time slows down or the room feels distant. A few report mild hallucinations-seeing shapes, hearing echoes, or feeling like they’re floating. These aren’t signs of psychosis. They’re direct effects of the drug on brain circuits. The good news? It doesn’t last. Dissociation usually peaks around 40 minutes after the spray and fades within 1.5 to 2 hours. By the fourth or fifth treatment, many patients say it’s much milder. One user on Reddit wrote: “My first session felt like I was watching myself from the ceiling. By session four, I just felt a little floaty for 20 minutes.” Clinics use a tool called the CADSS (Clinician-Administered Dissociative States Scale) to measure this. Scores above 3 mean severe dissociation-and that’s rare. Only 6.3% of patients hit that level. Still, every clinic is required to monitor it. No exceptions.Blood Pressure Spikes: The Hidden Risk
While dissociation gets most of the attention, blood pressure changes are just as critical. Esketamine causes a rapid, temporary rise in both systolic and diastolic pressure. On average, systolic pressure jumps 14-23 mmHg. Diastolic goes up 7-16 mmHg. That’s enough to trigger warning signs in people with heart conditions. In trials, 32.7% of patients had treatment-emergent hypertension-meaning their blood pressure climbed above 140/90. Compare that to 14.2% on placebo. It’s not just a number. For someone with untreated high blood pressure or a history of stroke, this could be dangerous. That’s why you can’t just show up and get sprayed. Before treatment, your blood pressure is checked. Then, every 5-10 minutes for the first 30-40 minutes. After that, every 15-30 minutes. If your pressure climbs too high-say, above 180/110-the session is stopped. You’re sent home. No exceptions. People with uncontrolled hypertension (BP over 160/100) are excluded from treatment. So are those with recent heart attacks, aneurysms, or brain malformations. These aren’t arbitrary rules. They’re based on real cases where unmonitored use led to serious outcomes.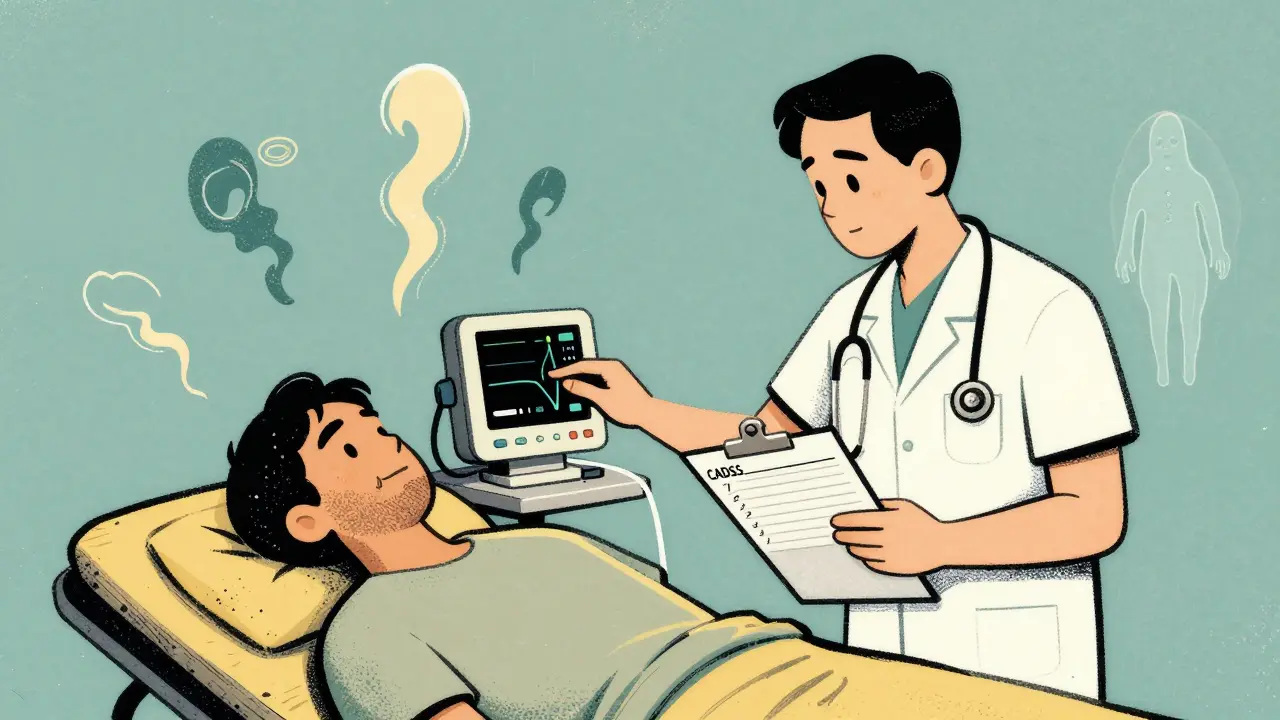
The REMS Program: Why You Can’t Take It Home
Esketamine is one of the few medications in the U.S. that requires a Risk Evaluation and Mitigation Strategy (REMS). That means you can’t get it from a pharmacy. You can’t self-administer. You must go to a certified clinic, sit in a monitored room, and stay for at least two hours after the spray. The process is rigid:- You arrive and check in.
- Your blood pressure, heart rate, and oxygen levels are taken.
- You’re given the spray-self-administered under staff supervision.
- You sit quietly in a dim, calm room for two hours.
- Staff check your vitals every 5-10 minutes.
- At 40 minutes, they assess dissociation using the CADSS.
- You can’t leave until the two hours are up, even if you feel fine.
What Patients Really Say
Real-world feedback paints a mixed picture. On Healthgrades, Spravato has a 3.7/5 rating. 62% of reviewers mention dissociation. 41% say it’s manageable. 21% call it severe-but still temporary. One patient wrote: “I cried during my first session because I felt so disconnected. But by week three, I was calm. And for the first time in years, I felt hope.” On the flip side, a user with pre-existing hypertension shared: “My systolic hit 170. They stopped the session. I had to quit. I’m not willing to risk a stroke for this.” The common thread? People who stayed in the program overwhelmingly credit the staff. “They knew exactly what to do,” said 91% of positive reviewers on Drugs.com. That’s not luck. It’s training.



this stuff is wild. i tried it. felt like i was floating through a wall. no joke. my brain just said 'bye' for an hour. glad they watch you like a hawk.
so you're telling me we're paying 10k per session for a drug that makes you feel like you're on acid but with more paperwork? classic america. also typo: 'spravato' is spelled 'spravato' in the article lol.
yo i'm from the philippines and we don't even have this. but i watched a vid of someone doing it in minneapolis. dude was giggling and crying at the same time. the staff looked like they were at a spa, not a medical facility. love how we're treating depression like a rave now. 🤪
i had a cousin do this. said the first time felt like his soul left his body. but after 3 sessions? he actually laughed again. not a joke. he hadn't in 7 years. the system sucks but it works. just wish it was cheaper.
the CADSS scale is legit. it's not just 'you feel weird.' it's quantified dissociation. i've seen the data. the fact that they log it every 5 mins? that's precision medicine. not magic. engineering.
they make it sound like a spa day but it's basically a chemical trip with a nurse watching you. also why do we need 2 hours? i felt fine after 20. :P
i know someone who had a stroke after doing this at home. that's why the rules are so strict. don't be that guy. just sit there. breathe. let it happen. it's not about comfort. it's about survival. <3
if you're not willing to sit for two hours you don't deserve to feel better. end of story. this isn't a coffee run. it's a medical procedure. get over it.
my aunt did this and said she saw her dead dog. not hallucination. she said she was talking to him. cried for 45 mins. then smiled. said she felt peace. i don't know if it's science or spirituality. but it worked.
Thank you for this comprehensive and meticulously detailed overview. The clinical rigor applied to esketamine administration is commendable, and the REMS framework reflects a robust commitment to patient safety. One might argue that such protocols are paradigm-shifting in psychiatric care delivery.
winnipeg here. we got one clinic. it's in a strip mall next to a tattoo parlor. weird combo. but the nurses? legends. one gave me a blanket and said 'you're safe here.' that's more than my therapist ever did.
makes me wonder if dissociation is just the brain saying 'enough' to all the noise. like it needs to shut down to reboot. maybe we're not fixing depression. just giving it a timeout.
this is so much work just to feel normal again. i'm tired.
the blood pressure spike is the real MVP here. no one talks about it. but if your BP hits 180/110 and they stop the treatment? that's not bureaucracy. that's someone refusing to let you die on a chair because you wanted to feel better. that's love in a white coat.
i think the real win isn't the drug. it's the fact that someone sat with you for two hours. no phone. no distractions. just presence. maybe that's the cure. the drug just opens the door.