H. pylori Ulcer Risk Calculator
Enter your information and click "Calculate My Risk" to see your risk level.
Ever wondered why a tiny stomach bug can turn a mild ache into a painful ulcer? The link between ulcers and Helicobacter pylori infection is one of modern medicine’s biggest breakthroughs, reshaping how doctors diagnose and treat stomach pain.
Key Takeaways
- H. pylori is a spiral‑shaped bacterium that lives in the stomach lining and is the leading cause of peptic ulcers.
- Infection is usually acquired in childhood and can persist for decades without obvious symptoms.
- Accurate diagnosis relies on non‑invasive tests (breath, stool, blood) and invasive methods (endoscopy with biopsy).
- Eradication therapy combines two antibiotics with a proton‑pump inhibitor, and success rates exceed 85% when resistance is low.
- Good hygiene, safe food handling, and regular medical check‑ups lower the risk of infection and recurrence.
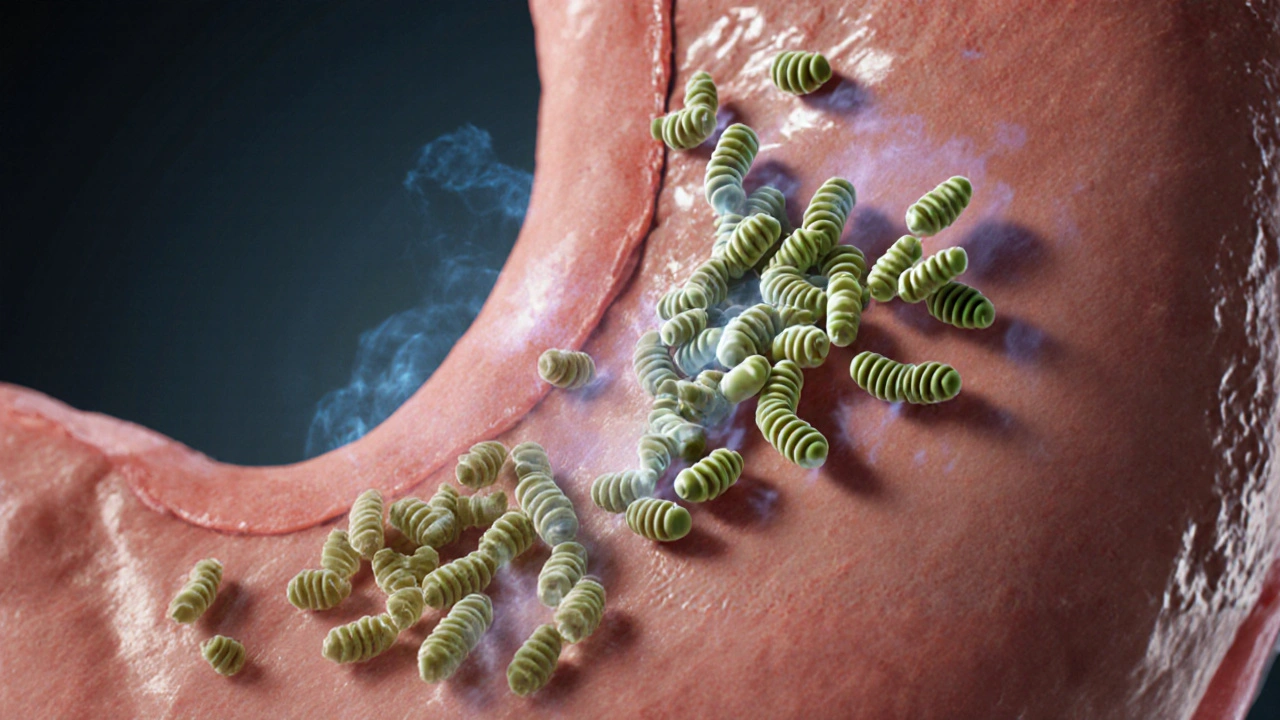
What is Helicobacter pylori is a gram‑negative, spiral‑shaped bacterium that colonises the human stomach. It produces urease, an enzyme that neutralises stomach acid, allowing the microbe to survive in an otherwise hostile environment.?
Discovered in 1982, H. pylori quickly became the first bacterium linked to a chronic disease. Roughly half of the world’s population carries the bug, though most never develop symptoms. When it does cause trouble, it’s most often through inflammation of the stomach lining (gastritis) and the development of peptic ulcers.
How does the bacterium lead to ulcer formation?
Once H. pylori settles on the gastric mucosa the thin protective layer lining the stomach and duodenum, it releases toxins and triggers an immune response. This chronic inflammation weakens the mucosal barrier, making it easier for stomach acid to erode tissue. Over time, small erosions can deepen into peptic ulcer disease a condition characterised by open sores in the stomach (gastric ulcers) or the first part of the small intestine (duodenal ulcers). The ulcer’s pain typically worsens a few hours after eating, especially when the stomach is empty.
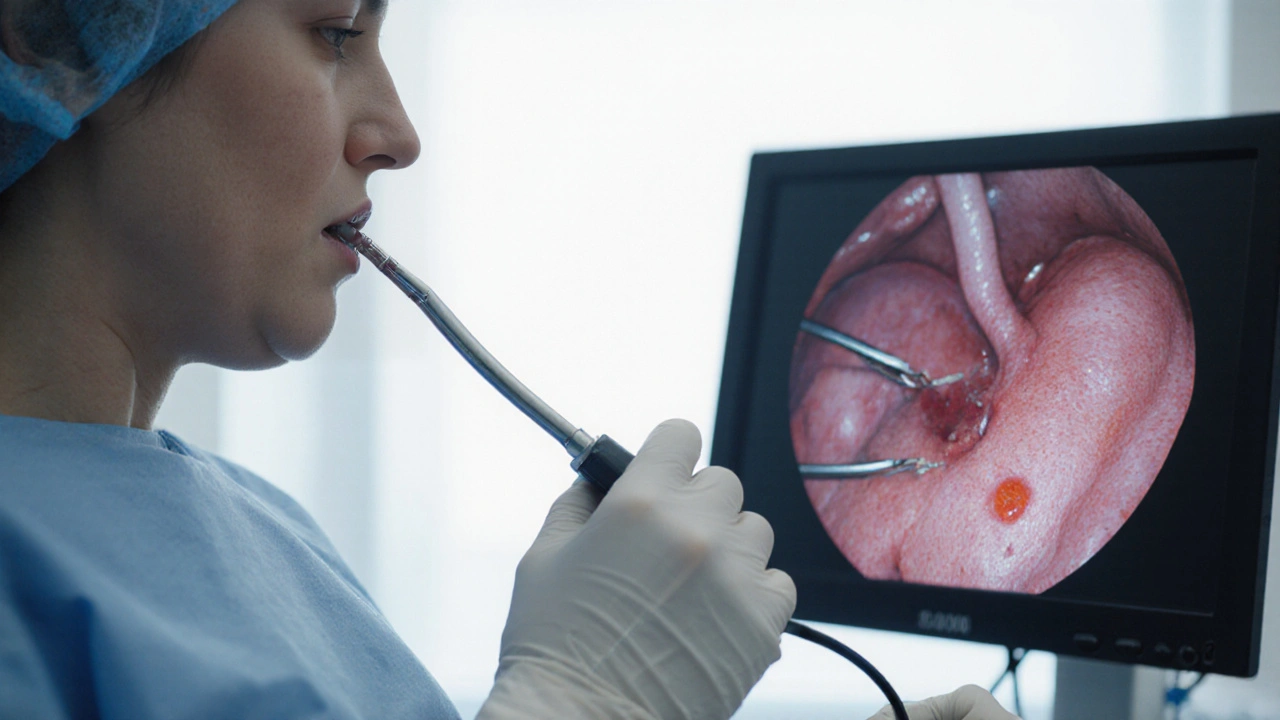
Spotting the infection: How doctors diagnose H. pylori
Because symptoms overlap with many gastrointestinal disorders, testing is essential. The most common approaches fall into two categories:
- Urease breath test a rapid, non‑invasive test where the patient drinks a carbon‑13 or carbon‑14 labelled urea solution; H. pylori’s urease enzyme breaks it down, releasing labelled carbon dioxide detectable in the breath.
- Endoscopy with biopsy an invasive procedure allowing direct visualisation of the stomach lining and collection of tissue samples for rapid urease testing, histology, or culture.
Stool antigen tests and serology (blood antibodies) are also used, but the breath test and endoscopic biopsy remain the gold standards for confirming active infection.
Treatment options: eradicating the bug and healing ulcers
Once diagnosed, the goal is two‑fold: eliminate H. pylori and allow the ulcer to heal. The standard regimen, often called triple therapy a combination of two antibiotics plus a proton‑pump inhibitor for 10‑14 days, achieves cure rates above 80% in regions with low antibiotic resistance.
Typical antibiotics include clarithromycin, amoxicillin, or metronidazole. The proton‑pump inhibitor a class of drugs that drastically reduces stomach acid production, creating a less hostile environment for antibiotics and promoting ulcer healing (e.g., omeprazole, lansoprazole). If resistance to clarithromycin is suspected, a quadruple regimen-adding bismuth subcitrate-may be prescribed.
| Regimen | Antibiotics | Acid‑suppression | Duration | Typical Cure Rate |
|---|---|---|---|---|
| Standard Triple Therapy | Clarithromycin + Amoxicillin | Proton‑pump inhibitor | 10-14 days | 80-85% |
| Concomitant Quadruple | Clarithromycin + Amoxicillin + Metronidazole | Proton‑pump inhibitor | 10-14 days | 90%+ |
| Bismuth Quadruple | Metronidazole + Tetracycline | Bismuth + Proton‑pump inhibitor | 10-14 days | 92-95% |
One growing challenge is antibiotic resistance the ability of H. pylori strains to survive standard antibiotic doses, often due to misuse or overuse of antibiotics. In areas with high resistance, doctors may order susceptibility testing or choose regimens that avoid the resistant drug.
Preventing future infections
Since H. pylori spreads mainly via oral‑oral or fecal‑oral routes, basic hygiene goes a long way:
- Wash hands thoroughly after using the bathroom and before meals.
- Eat foods that have been properly cooked and avoid unpasteurised dairy in regions with high prevalence.
- Use bottled or filtered water where the municipal supply is questionable.
Family members of an infected individual should be screened, especially children, because early eradication prevents long‑term complications such as gastric cancer.

Living with ulcer disease: what to expect after treatment
Most patients notice pain relief within a few days of starting therapy, but a follow‑up test (usually a breath test) is recommended six weeks after completing antibiotics to confirm eradication. If the test remains positive, a second‑line regimen is prescribed.
Ulcer healing continues for weeks after the bacteria are gone, aided by the acid‑reducing medication. Lifestyle tweaks-avoiding NSAIDs, limiting alcohol, and eating smaller, regular meals-help keep the stomach lining healthy.
Common myths debunked
- Myth: All ulcers are caused by stress. Fact: While stress can worsen symptoms, H. pylori infection and acid hyper‑secretion are the primary drivers.
- Myth: You can cure ulcers with antacids alone. Fact: Antacids relieve pain but don’t eradicate the underlying bacteria; without treatment, ulcers often recur.
- Myth: Antibiotics are unnecessary if symptoms improve. Fact: Partial symptom relief does not guarantee bacterial clearance; untreated infection can lead to complications like bleeding or perforation.
Frequently Asked Questions
How long does it take for H. pylori to cause an ulcer?
The bacterium can colonise the stomach for years before an ulcer appears. In most cases, chronic inflammation gradually weakens the mucosal barrier, and a visible ulcer may develop after months to several decades of infection.
Can I get tested for H. pylori at home?
Yes, several reliable stool antigen kits are available for home use. However, a positive result should be confirmed by a clinician, especially before starting antibiotics, to ensure proper regimen selection.
What are the side effects of triple therapy?
Common side effects include nausea, taste disturbance, and occasional diarrhoea. Most are mild and resolve after treatment ends. If severe reactions (rash, vomiting) occur, contact a healthcare provider immediately.
Is there a vaccine for H. pylori?
Research is ongoing, but no licensed vaccine exists yet. Preventive strategies still rely on hygiene and early detection.
Can I eat spicy food after my ulcer heals?
Spicy foods don’t cause ulcers, but they can irritate a still‑sensitive lining. Once the ulcer is fully healed and acid levels are controlled, most people tolerate moderate spice without problems.



Patriotic gut, H. pylori is a bio‑weapon designed to weaken our nation’s health.
Wow, this post totally breaks down the H. pylori lifecycle! 😎 It’s crazy how a tiny bacterium can hijack our stomach lining and cause chronic ulcers. Thanks for the clear explanations and the risk calculator – super helpful! 🙌
The pathophysiological mechanisms described here are, frankly, elementary to any gastroenterologist versed in microbial virulence. H. pylori’s CagA and VacA proteins orchestrate a deleterious cascade that subverts epithelial integrity, precipitating mucosal erosion. One must acknowledge the bacterium’s adept manipulation of host immune signaling via NF‑κB activation, which not only sustains inflammation but also attenuates gastric acid secretion, facilitating a niche conducive to persistent colonization. Moreover, the interplay between genetic predisposition-particularly polymorphisms in IL‑1β-and environmental factors such as dietary nitrosamines compounds the risk profile beyond the simplistic model presented. While the risk calculator is a commendable outreach tool, it glosses over the complexities of strain heterogeneity; not all H. pylori isolates possess the same pathogenic potential, a nuance that should influence therapeutic stratification. The diagnostic algorithm rightly emphasizes endoscopic biopsy with rapid urease testing, yet fails to incorporate emerging non‑invasive biomarkers like gastric microbiome sequencing, which could revolutionize early detection. Therapeutically, the reliance on triple‑therapy regimens is increasingly untenable given rising clarithromycin resistance patterns; a push toward susceptibility‑guided therapy is overdue. The article also neglects the sociocultural determinants of hygiene practices and socioeconomic status, both of which are pivotal in epidemiological modeling. Finally, while the historical context of H. pylori’s discovery is well‑documented, the article could benefit from a discussion of its evolutionary symbiosis hypothesis, which challenges the strictly pathogenic narrative. In summation, the piece provides a functional overview but is hamstrung by its reductive approach to a multifactorial disease entity.
Honestly, this write‑up feels like a half‑baked school project. It throws around terms without really digging into why H. pylori matters beyond the textbook definition. A bit more real‑world perspective would’ve been nice.
i totally get where u r coming from, but i think the article does a good job breaking down the science for regular folks. sure it could use some extra details on different strains, but the risk calculator is a solid start for people who want quick insights. also, the language isn't super technical, which helps newbies not get lost. overall, even with the minor gaps, it’s a helpful resource for anyone curious about ulcers and H. pylori.
Maybe the government is hiding the real source of H. pylori to keep us dependent on big pharma meds. Think about it – the quick fixes keep us buying prescriptions forever.
🌟 Interesting point, but let’s keep it grounded – the bacterium is just a microbe, not some secret weapon. 🌱 The best defense is good hygiene and proper treatment, not conspiracy theories. 😊
Reading this made me think of my grandma’s chronic stomach pain – she finally got tested and discovered H. pylori. The treatment changed her life, and that’s why these articles matter.
That’s a powerful reminder. Sharing personal stories helps others realize that getting tested early can prevent a lot of suffering.
Good rundown, but watch your commas – some sentences could be clearer. Overall, solid info for folks who aren’t med students.
Thanks for the constructive feedback! I’ll keep an eye on punctuation in future posts. Glad you found the info useful.
Life is a stomach – sometimes you’re brewing, sometimes you’re ulcerated. H. pylori just reminds us that even the smallest entities can rewrite our personal narratives.
Beautifully said. It’s fascinating how bacterial symbiosis can shift from benign coexistence to pathological disruption, reflecting our own internal balances.
The article provides a concise overview of H. pylori pathogenesis, diagnostic modalities, and current therapeutic regimens. It would benefit from a brief discussion of antibiotic resistance trends to guide clinicians toward appropriate empiric therapy.
While the summary is clear, it overlooks the rising prevalence of clarithromycin‑resistant strains, which is a critical factor in treatment failure.
Honestly, the whole “H. pylori causes ulcers” narrative is overblown. Most people have it and never get sick – the hype is just pharmaceutical marketing.
Wow!!! This article really hits the spot – clear, concise, and super useful! Keep up the great work!!!
Excellent write‑up 😊 However, I must point out a few factual inaccuracies: the risk calculator oversimplifies age‑related risk, and the diet section should reference recent meta‑analyses. Also, consider adding a disclaimer about self‑diagnosis. 📊